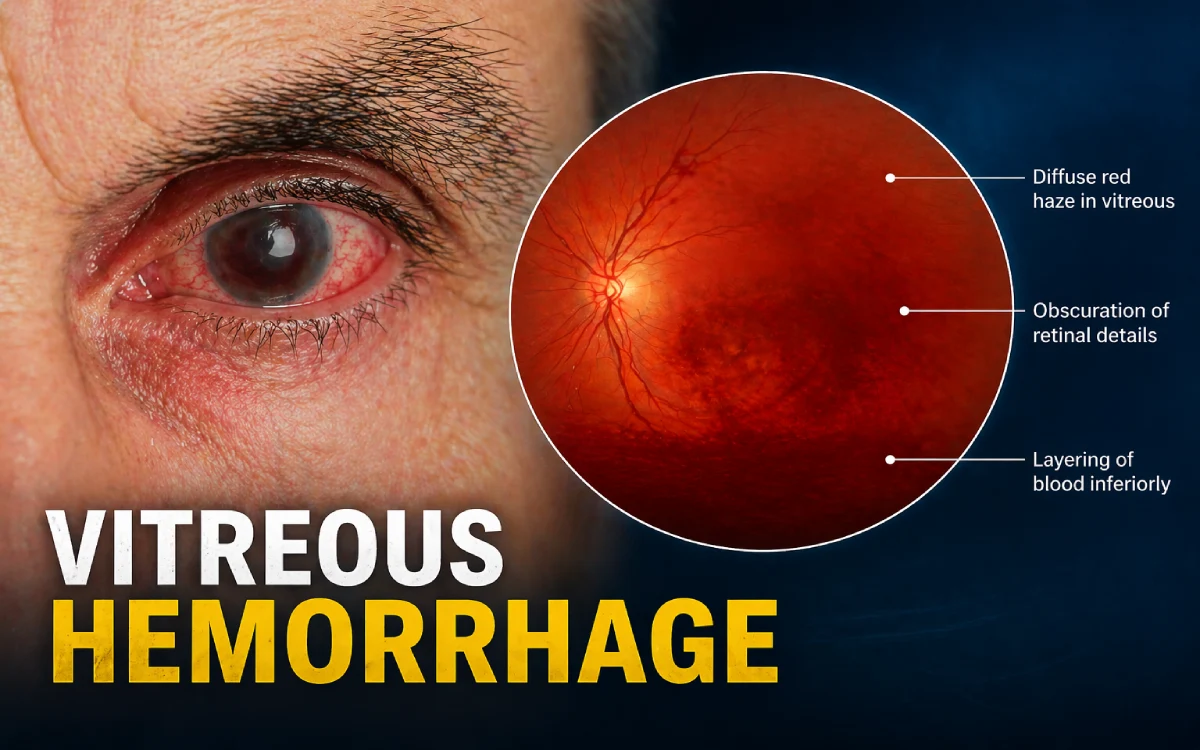
Imagine waking up to dozens of dark cobwebs, smoky haze, or a reddish curtain drifting across your vision, all without any pain. This sudden, alarming change is often the first sign of vitreous hemorrhage, a condition where blood leaks into the clear, gel-like vitreous that fills the center of your eye.
While it sounds scary, the good news is that timely evaluation by a retina specialist can often preserve or restore vision. Many cases improve with proper care, and modern treatments have made outcomes better than ever.
What Is Vitreous Hemorrhage?
The vitreous is a transparent, jelly-like substance that helps maintain the eye’s shape and allows light to reach the retina (the light-sensitive layer at the back of the eye). When blood vessels leak into this space, light scatters or gets blocked, causing blurred, hazy, or patchy vision.
Vitreous hemorrhage is not usually a disease on its own it’s often a symptom of an underlying issue in the retina or blood vessels. The amount and location of blood determine how severely vision is affected.
Common Symptoms: What Patients Typically Notice
Symptoms usually appear suddenly and painlessly in one eye:
- New or sudden increase in floaters (dots, strings, cobwebs, or soot-like spots)
- Blurred, foggy, or hazy vision
- Reddish or brownish tint to vision
- Difficulty reading, recognizing faces, or seeing clearly
- Shadows or a “curtain” effect in the side vision
- Flashes of light (especially if the retina is being tugged)
Mild bleeds may feel like mild floaters, while dense ones can reduce vision dramatically, sometimes to just perceiving light and dark.
Important: These symptoms deserve prompt attention, even if they seem mild at first.
Main Causes of Vitreous Hemorrhage
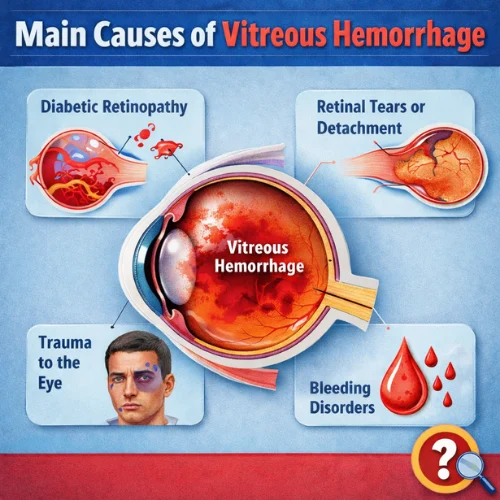
Several conditions can trigger bleeding into the vitreous. The most common include:
- Proliferative Diabetic Retinopathy — Weak, abnormal new blood vessels on the retina bleed easily. This remains one of the leading causes, especially in working-age adults.
- Posterior Vitreous Detachment (PVD) with or without Retinal Tear — As we age, the vitreous shrinks and pulls away from the retina. This can tear small vessels or the retina itself.
- Retinal Tear or Detachment — Traction on the retina can rupture blood vessels; untreated tears risk full detachment and permanent vision loss.
- Eye Trauma — Blunt or penetrating injuries (sports, falls, accidents) are a frequent cause, particularly in younger people.
- Retinal Vein Occlusion — Blockage in a retinal vein raises pressure and can cause leakage.
- Other Causes — High blood pressure, inflammation, blood disorders (e.g., sickle cell), age-related macular degeneration, or rarely tumors.
In many adults, diabetic retinopathy and PVD-related issues together account for the majority of cases.
Who Is at Higher Risk?
You have an elevated risk if you have:
- Diabetes (especially if poorly controlled)
- High blood pressure or vascular disease
- High myopia (very short-sightedness)
- History of eye injury or previous retinal surgery
- Blood-thinning medications or clotting disorders
Regular retinal screenings are especially important for these groups.
Risks If Left Untreated
The biggest danger isn’t always the blood itself; it’s the underlying cause. A hemorrhage may hide a retinal tear or detachment that can lead to permanent vision loss if not addressed quickly. Other risks include recurrent bleeding, scar tissue formation (traction), or complications like ghost cell glaucoma.
Early assessment prevents these issues and improves the chances of full recovery.
When to Seek Urgent Care
Treat new or sudden vision changes as an emergency. Seek immediate retinal evaluation if you experience:
- Sudden increase in floaters or flashes
- Blurred or lost vision in one eye
- A dark shadow or curtain in your peripheral vision
- Recent eye trauma
- Known diabetes or high-risk conditions
Prompt diagnosis can make the difference between observation and more intensive treatment.
How Doctors Diagnose Vitreous Hemorrhage
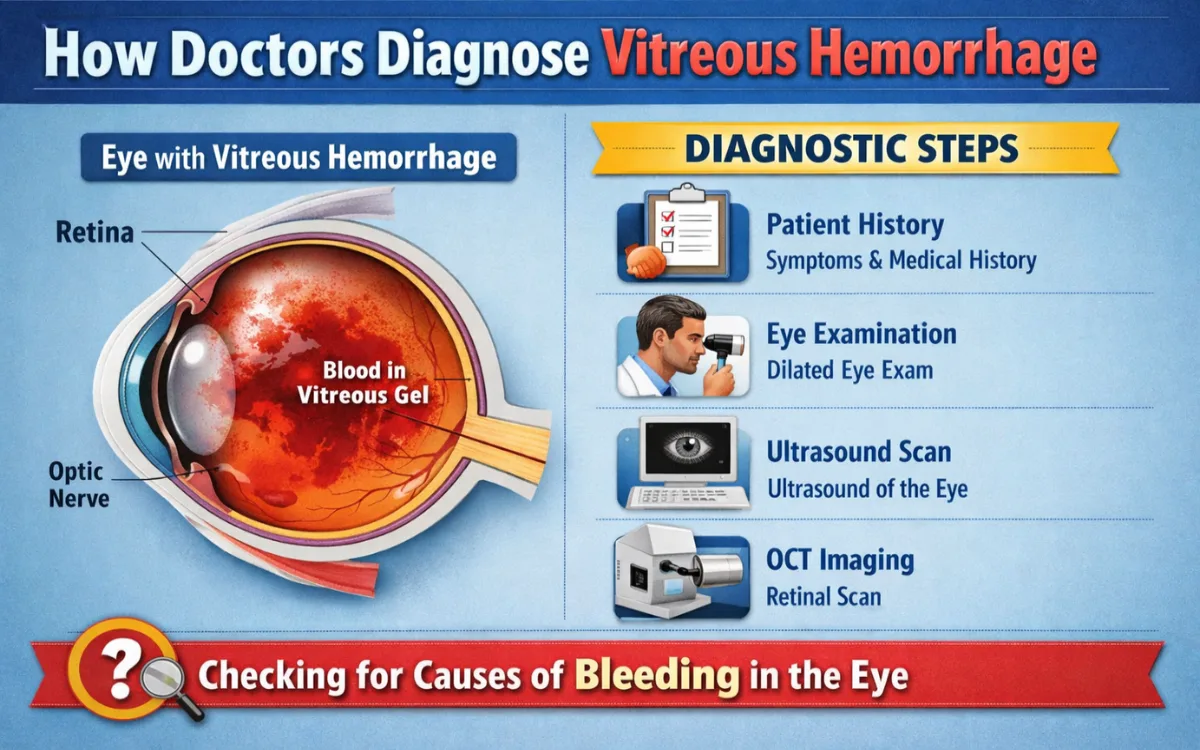
Diagnosis starts with a detailed history and dilated retinal exam. If blood obscures the view:
- Ocular Ultrasound (B-scan) — Safely images the retina behind the blood to check for tears, detachment, or other problems.
- Additional imaging (OCT, fluorescein angiography) will be performed once the view clears.
These tools allow precise identification of the cause.
Modern Treatment Options
Treatment is tailored to the cause, severity, and stability of the retina.
- Observation — Small bleeds with an intact retina often clear naturally over weeks to months. Close monitoring is essential.
- Laser Photocoagulation — Seals abnormal vessels, especially in diabetic cases, to prevent further bleeding.
- Intravitreal Injections (Anti-VEGF) — Medications injected into the eye reduce abnormal vessel growth and leakage. Often used before surgery in diabetic cases to make the procedure safer and improve outcomes.
- Vitrectomy Surgery — For dense, persistent, or recurrent hemorrhage (or when a tear/detachment is present). Surgeons remove the blood-filled vitreous and replace it with a clear solution.
Modern small-gauge (25- or 27-gauge) vitrectomy uses tiny incisions, resulting in faster recovery, less discomfort, and higher precision. In many cases, vision improves significantly once the blood is cleared and the underlying issue is fixed. Success rates for clearing the hemorrhage are very high (often 90%+ with timely intervention).
What Recovery Looks Like
Recovery varies:
- Mild cases may improve gradually as blood absorbs.
- After vitrectomy, many patients notice clearer vision within days to weeks, though full stabilization can take 1–3 months.
- Outcomes depend on the health of the retina and how quickly treatment begins. Timely care often prevents further damage and restores functional vision.
Your doctor will guide activity restrictions, follow-up visits, and signs to watch for.
Can Vitreous Hemorrhage Be Prevented?
Not every case is preventable, but you can lower your risk by:
- Keeping diabetes, blood pressure, and cholesterol well-controlled
- Attending regular dilated eye exams (especially if high-risk)
- Wearing protective eyewear during sports or hazardous work
- Seeking immediate care for any new flashes, floaters, or vision changes
Patient awareness and proactive check-ups remain the best defense.
Vitreous Hemorrhage Treatment in Dubai
In Dubai, patients benefit from advanced retinal diagnostics, including high-resolution imaging and micro-incision vitrectomy techniques. If you’re experiencing sudden floaters, blurred vision, or other symptoms, rapid assessment by an experienced retina specialist is crucial to identify the cause and choose the safest treatment path, whether monitoring, laser, injections, or surgery.
Experiencing symptoms? Don’t wait. Contact Dr. Mandeep Lamba at +971 50 407 2552 at Prime Hospital, Al Garhoud, Dubai, for expert evaluation and personalized care.
Frequently Asked Questions
1. Is vitreous hemorrhage always an emergency?
Not every case requires immediate surgery, but every new case needs prompt specialist assessment to rule out serious underlying problems.
2. Can the blood clear on its own?
Yes, many mild bleeds resolve gradually over weeks to months. However, this does not replace the need for a full retinal check.
3. Is it painful?
Usually painless. Most people only notice visual symptoms.
4. Will surgery restore normal vision?
In many cases, yes especially if the retina is healthy and treatment is timely. Results depend on the underlying condition and any prior retinal damage.
5. Can diabetes cause it without other symptoms?
Yes. Significant retinal changes can develop silently before a bleed occurs.
Conclusion
Do not mistake vitreous hemorrhage for “just floaters.” It can be an early warning sign of a serious retinal problem, including diabetic retinopathy, a retinal tear, or even retinal detachment. The good news is that with early diagnosis and timely treatment, most patients can protect their vision and avoid long-term complications.
If you notice sudden floaters, flashes, blurred vision, or unusual visual changes, do not wait. Contact Dr. Mandeep Lamba on +971 52 422 7000 at Prime Hospital, Al Garhoud, Dubai, for prompt retinal assessment and expert treatment.