A red eye is easy to ignore. Most people blame it on screen time, lack of sleep, dust, or simple irritation. And sometimes, that is true. But when the redness keeps coming back, stays for days, or becomes something you notice almost every morning, it is no longer just a minor cosmetic issue. It is often your eyes’ way of telling you that something is not right.
That is where chronic red eye becomes important. What looks like “just redness” can actually come from very different causes, from dryness and allergies to eyelid inflammation, contact lens irritation, corneal problems, or even deeper inflammation inside the eye.
The mistake many people make is trying to self-treat it without understanding the real cause. And that is exactly why persistent redness should never be dismissed.
Why a Red Eye Should Not Be Judged by Colour Alone
Patients naturally focus on what they can see in the mirror. Doctors look beyond the colour and ask a different set of questions. Is it itchy? Is it painful? Is vision affected? Is one eye worse than the other? Does it come with discharge, burning, dryness, light sensitivity, or headache?
That matters because two eyes can look similarly red but have completely different causes. The American Academy of Ophthalmology notes that red, watery, or swollen eyes are not always conjunctivitis and may also be caused by dry eye, allergies, blepharitis, uveitis, or glaucoma.
When Redness Becomes a Pattern
A short episode of irritation may settle on its own. But when the problem lasts, repeats often, or becomes part of daily life, it deserves more than a temporary fix. Many people keep reaching for over-the-counter drops because they want the eye to look better quickly. The difficulty is that a red eye is a symptom, not a diagnosis.
In a clinic, the goal is not simply to make the eye look whiter. The real aim is to find out what is driving the irritation. That could be a tear film problem, an eyelid issue, an allergy, an infection, a contact lens complication, or inflammation deeper inside the eye. This is why chronic red eyes should be approached with proper examination rather than repeated self-treatment.
Common Causes of Long-Standing Eye Redness
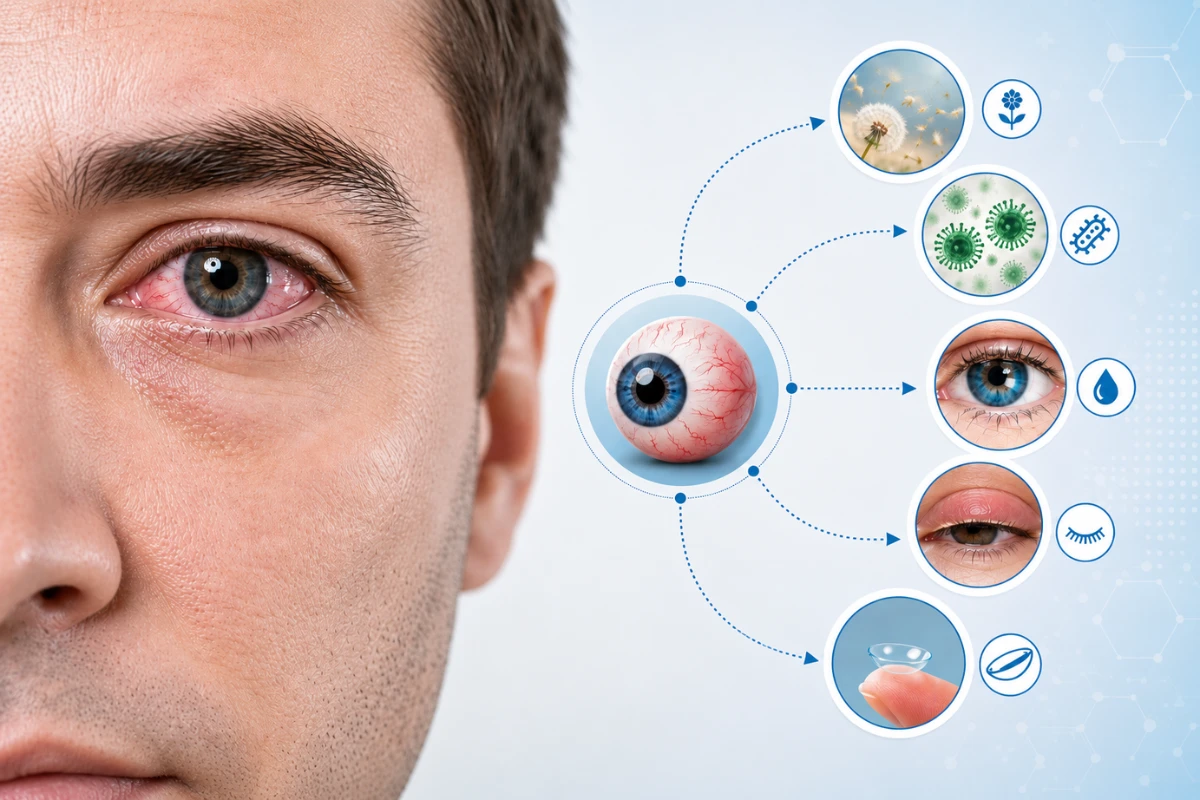
Not every persistent red eye means something dangerous. In fact, many causes are manageable once correctly identified. The challenge is that they can overlap and often look similar to the patient.
Dry Eye Disease
Dry eyes are one of the most common reasons for ongoing redness. The eye needs a stable tear film to stay comfortable and clear. When that tear film breaks down, the surface becomes irritated and inflamed, leading to redness, grittiness, burning, and fluctuating discomfort. Dry eye is associated with ageing, certain medications, medical conditions, air-conditioned environments, and prolonged screen use, which reduces blinking.
Allergic Eye Disease
Allergy is another very common cause, especially in people who also have sneezing, eczema, hay fever, or dust sensitivity. The classic clue is itching. Redness is often present in both eyes and usually comes with watering and frequent rubbing. Mayo Clinic notes that allergies are a common cause of red eyes, and allergic eye disease often affects both eyes rather than only one.
Blepharitis and Eyelid Margin Disease
Sometimes the redness does not begin in the eyeball itself. It begins at the eyelids. When the eyelid margins are inflamed or the oil glands do not function properly, the tear film becomes unstable, and the eye surface becomes irritated. Patients often describe burning, crusting, sticky lashes in the morning, and a tired or heavy feeling in the eyes. The AAO notes that blepharitis is commonly seen in practice and often contributes to dry eye symptoms.
Conjunctivitis
Conjunctivitis is the cause many people think of first, but it is only one part of the picture. Viral conjunctivitis often causes watering and may follow a cold. Bacterial conjunctivitis is more likely to produce thicker discharge. Allergic conjunctivitis usually itches more than it hurts. NHS guidance also highlights that pain, light sensitivity, or vision changes suggest that the problem may be more serious than simple conjunctivitis.
Contact Lens-Related Problems
A red eye in a contact lens wearer should always be taken more seriously. The cause may be dryness, overwear, poor hygiene, or surface irritation, but lens wear also increases the risk of corneal infection. When redness is paired with pain, light sensitivity, or blurred vision in a contact lens user, the cornea must be checked carefully.
Corneal Disease
The cornea is the clear front window of the eye. When it becomes inflamed or infected, symptoms are usually more intense. Keratitis can cause redness, pain, watering, blurred vision, discharge, and sensitivity to light. These are not symptoms to sit on for days, hoping they disappear.
Deeper Inflammation or Eye Disease
This is where doctors become more cautious. Conditions such as uveitis, scleritis, and glaucoma can also present with redness, but they usually come with warning signs like pain, photophobia, reduced vision, headache, or a very deep-looking redness. NHS guidance on uveitis and glaucoma makes clear that red eyes associated with pain or visual symptoms need urgent review.
Understanding Allergy and Infection More Clearly
One of the most common questions patients ask is whether their redness sounds more like an allergy or an infection. That confusion is understandable because symptoms can overlap. Looking at the pattern often helps more than looking at the redness itself.
When thinking about red eyes allergy vs infection, allergy usually leans more toward intense itching, both eyes being involved, watering more than sticky discharge, and symptoms that flare after dust, pollen, pets, or seasonal triggers. Infection is more likely when one eye starts first, discharge becomes more obvious, the eyelids stick together on waking, or there has been a recent cold or viral illness. Even then, home guessing is not always reliable because dry eye, blepharitis, and viral irritation can all mimic one another.
Why Specialists Think More Broadly Than “Just Pink Eye”
Persistent redness is not assessed as a single label. Specialists work through a wider list of possibilities. That process may include dryness, eyelid inflammation, allergy, viral or bacterial conjunctivitis, corneal disease, uveitis, scleritis, lens-related complications, or glaucoma. The AAO specifically warns that not every red eye is conjunctivitis and that atypical or persistent cases need careful evaluation. That broader approach is what doctors mean when they consider a chronic red eye differential diagnosis, rather than jumping to one assumption too early.
Symptoms That Raise Concern
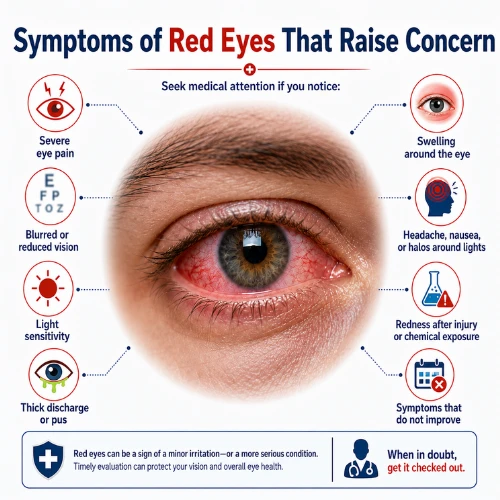
Redness alone does not always mean an emergency. Redness plus certain symptoms is what changes the level of concern.
Doctors become more cautious when redness is associated with:
- eye pain
- sensitivity to light
- blurred or reduced vision
- marked one-sided symptoms
- severe headache
- Contact lens use with pain
- an irregular pupil
- a very dark red appearance
- recent trauma or something entering the eye
NHS emergency guidance advises urgent assessment for red eyes that come with severe pain, photophobia, visual changes, contact lens-related infection risk, headache, or pupil changes.
This is exactly when to worry about chronic red eyes: not only when the eye looks red, but when the redness stays, returns repeatedly, or begins to travel with pain, blurred sight, or light sensitivity.
How an Ophthalmologist Evaluates Persistent Redness
Many patients assume the consultation is only about checking for infection. In reality, the examination is much more detailed than that.
From a persistent red eye ophthalmology point of view, the specialist wants to know whether the source of irritation is mainly at the lids, the tear film, the conjunctiva, the cornea, or deeper inside the eye. That usually involves a focused history, slit-lamp examination, eyelid and tear assessment, and in selected cases, pressure testing or further investigations. The examination helps separate surface irritation from corneal disease, inflammation, or pressure-related problems that need a different treatment plan.
Why Whitening Drops Are Not a Real Solution
This is one of the commonest mistakes patients make. Redness-relieving drops can temporarily shrink surface blood vessels, so the eye may look better for a few hours. But they do not treat the underlying cause. In some people, repeated use can even lead to rebound redness, where the eye looks redder again later. The AAO advises that cosmetic redness drops can mask the problem without solving it, and they should never replace a proper diagnosis when symptoms persist.
If the real issue is dryness, allergy, blepharitis, corneal irritation, or deeper inflammation, the treatment needs to match that cause rather than simply hiding the redness.
Treatment Depends on the Cause
This is why a correct diagnosis matters so much. A red eye caused by dryness needs a different plan from one caused by allergy or infection. If the problem is dryness, treatment may focus on lubricants, eyelid care, screen habit changes, and improving the tear film. If allergy is driving the redness, avoiding triggers and using the right anti-allergy drops becomes more helpful than repeated rubbing. If eyelid disease is involved, warm compresses and lid hygiene often play an important role. If infection, corneal disease, or deeper inflammation is present, treatment becomes more specific and sometimes more urgent.
The key message is simple: redness is visible, but the real problem may be invisible without a proper eye examination.
FAQs
Can screen time cause long-lasting red eyes?
Yes. Long hours on screens reduce blink rate, which can destabilise the tear film and worsen dryness-related redness.
Are both eyes usually red in an allergy?
Often, yes. Allergy commonly affects both eyes and is usually associated with itching and watering.
Is sticky discharge always a bacterial infection?
No. Viral eye conditions can also produce discharge, and the full symptom pattern matters more than one sign by itself.
Can dry eye really look as red as an infection?
Yes. Dry eye can create significant surface inflammation and visible redness.
Should I use antibiotic drops just in case?
No. Using treatment without knowing the cause can delay the right diagnosis and may not help at all. Persistent symptoms need proper assessment.
Conclusion
A red eye that keeps coming back is not something to keep masking with random drops and guesswork. In many cases, the solution is straightforward once the real cause is identified, whether that is dryness, allergy, eyelid inflammation, infection, or a deeper eye condition. The important step is not to keep chasing temporary relief, but to get the eye examined properly so the treatment actually matches the problem.
If your eye redness has become frequent, stubborn, or is starting to affect comfort, vision, or daily life, the next step is a specialist evaluation. For expert eye assessment in Dubai, contact Dr Mandeep Lamba on +971 52 422 7000 and get a clear diagnosis, the right treatment plan, and the reassurance of knowing exactly what your eyes need.




